History:
A patient in their mid-30’s with no PMH is BIBA for episodic dizziness and chest pain and nausea both yesterday and today. The pain was 9/10 but is now gone after 0.4 SL nitro. He denies SOB or other complaints
Exam:
Vital signs are normal except for bradycardia. Physical exam is unremarkable
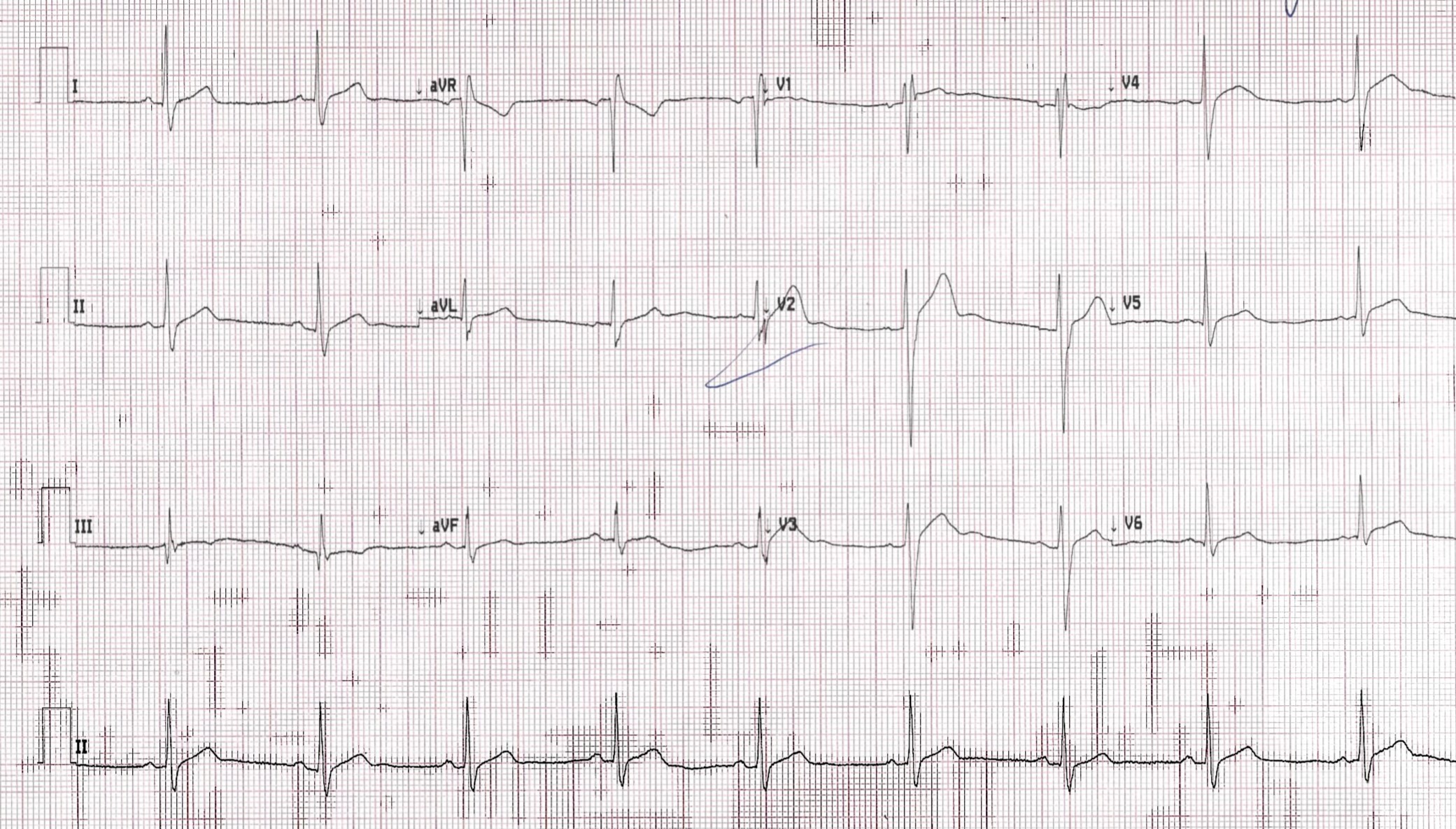
An ECG is done
Computer Read: SB at 55, IRBBB, ST elevation c/w injury, pericarditis or BER. There was no old ECG available for comparison but a repeat ECG was unchanged.
What is the most likely cause of the ECG findings in this patient?
- A) Anxiety/Panic
- B) Blood clot (PE)
- C) Cardiac: ACS
- D) Pericarditis
- E) Electrolyte issue
<<<<<<<<<<<<<<<<<<<<< ADVERTISEMENT & SPACER >>>>>>>>>>>>>>>>>>>>>
THE EMERGENCY MEDICINE POCKETBOOK TRIFECTA

Emergency Medicine 1-Minute Consult, 5th edition
A-to-Z EM Pharmacopoeia & Antibiotic Guide, NEW 5th edition (currently printable pdf only)
8-in-1 Emergency Department Quick Reference, 5th edition
******************************************************************************
<<<<<<<<<<<<<<<<<<<<<<<<< END SPACER >>>>>>>>>>>>>>>>>>>>>>>>>
ECG ANALYSIS, QUIZ ANSWER, CASE OUTCOME/PEARLS & 1-MINUTE CONSULT:
My ECG interpretation (by Dr. D. Brady Pregerson of ERpocketbooks.com): there is no PR depression. There is anterior and lateral ST elevation without reciprocal changes. There is no real ST elevation inferiorly but there is a positive Spodik’s sign anteriorly although one could argue it also looks like there is a U-wave.
QUIZ ANSWER: What is the most likely cause of the ECG findings in this patient?
- A) Anxiety/Panic
- B) Blood clot (PE) – can certainly occur with bradycardia but fits pericarditis better and D-dimer negative
- C) Cardiac: ACS – serial trops were negative
- D) Pericarditis – CORRECT
- E) Electrolyte issue
1-Minute Consult on this topic: Click HERE and scroll to proper page
Case Outcome: CBC metabolic panel essentially normal except for bicarb of 19 with normal anion gap. Troponin normal – repeat not indicated due to duration of pain. Chest x-ray normal. CT for rule out dissection shows no neither dissection nor PE.
Patient symptoms and ECG findings most concerning for pericarditis. Cardiology consulted and recommended discharge home with colchicine.